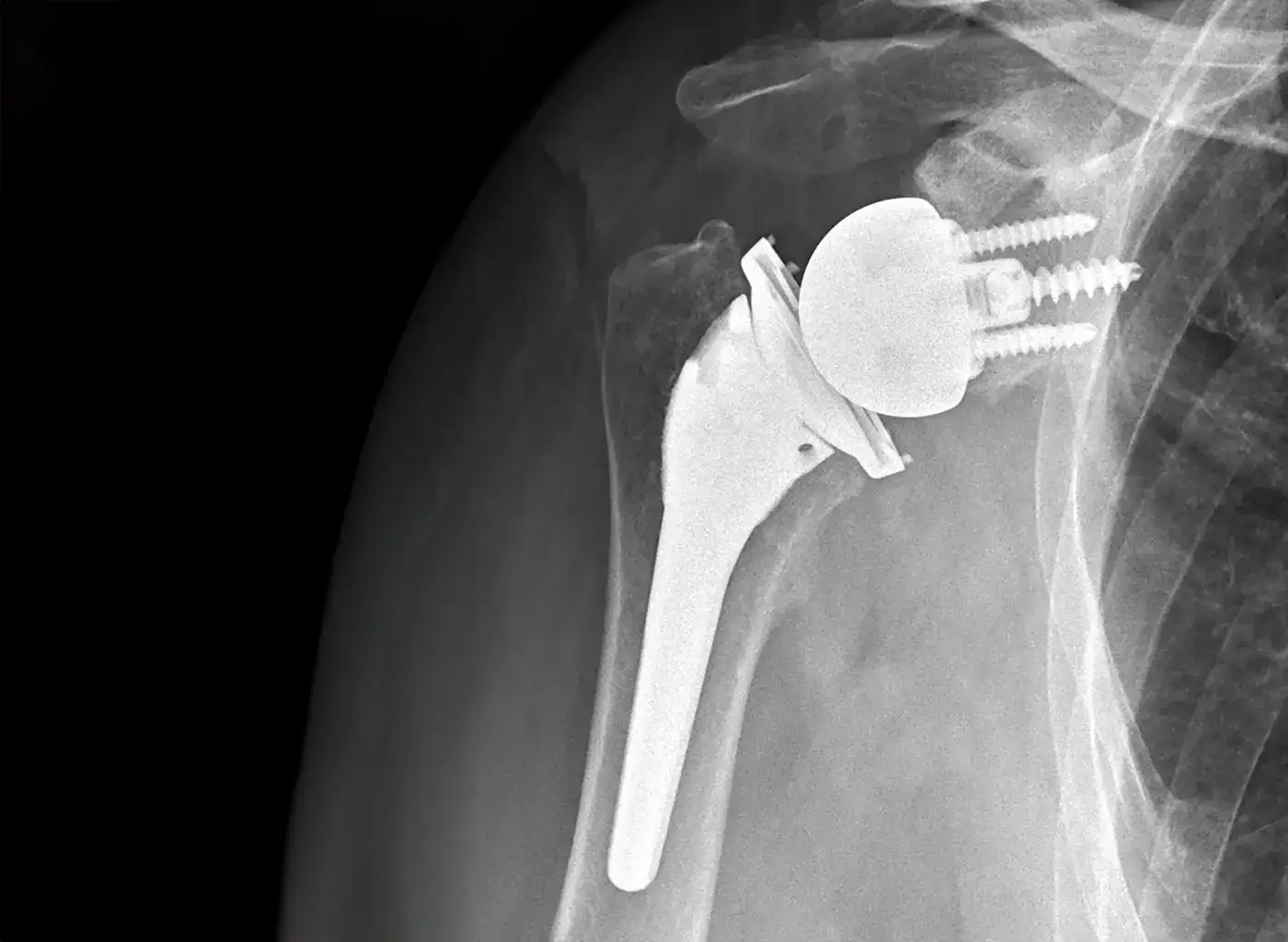
Reverse Shoulder Replacement
Mark A. Schrumpf, MD | Northern California's Orthopedic Surgeon
Understanding Reverse Shoulder Replacement
When chronic shoulder pain and loss of function begin to interfere with daily life, many patients turn to advanced surgical solutions. One such procedure is the reverse shoulder replacement, a specialized surgery designed for individuals with severe shoulder damage, especially when the rotator cuff is no longer repairable. Understanding how this procedure works, when it is recommended, and what recovery entails is an important step toward restoring mobility and relieving pain.
What is Reverse Shoulder Replacement?
The shoulder is a ball-and-socket joint. In a healthy shoulder, the “ball” (the head of the humerus, or upper arm bone) fits into the “socket” (the glenoid, a part of the shoulder blade). A network of muscles and tendons, known as the rotator cuff, stabilizes this joint and powers its movement.
A traditional total shoulder replacement mimics this natural anatomy. It replaces the humeral head with a metal ball and the glenoid socket with a plastic cup. However, this design generally relies on a healthy, functional rotator cuff to work correctly.
Reverse shoulder replacement, or reverse total shoulder arthroplasty, fundamentally changes this anatomy by “reversing” the position of the ball and socket. The surgeon attaches a metal ball to the shoulder blade (glenoid) and a plastic socket to the top of the humerus. This innovative design changes the biomechanics of the shoulder and allows the deltoid muscle, which covers the shoulder, to take over the function of the damaged rotator cuff. This shift in mechanics may restore movement and relieve pain, even when the rotator cuff is severely compromised.
When May Reverse Shoulder Replacement Be Recommended?
The primary goal of reverse shoulder replacement is to alleviate pain and improve the ability to lift the arm. This procedure is typically reserved for patients who have exhausted non-surgical options and whose shoulder pathology meets specific criteria. The most common indications for this surgery include:
- Cuff Tear Arthropathy: A severe form of shoulder arthritis that develops after a long-standing rotator cuff tear. Without the rotator cuff to center the humeral head, the ball migrates upward. This upward migration causes the humeral head to rub against the acromion, the bone at the top of the shoulder blade.
- Complex Shoulder Fractures: In certain severe, complex fractures of the upper humerus, especially in older patients with poor bone quality, the blood supply to the bone fragments may be compromised.
- Irreparable Rotator Cuff Tears: Some patients have massive rotator cuff tears that cannot be surgically repaired. These tears lead to chronic pain and significant weakness, particularly the inability to raise the arm.
- Chronic Dislocation: If the joint is too unstable and the surrounding soft tissues are too damaged, the reverse design can provide stability.
Preparing for Reverse Shoulder Replacement Surgery
Preparation is an important component of a successful surgical outcome. Patients who prepare thoroughly may experience smoother surgeries and recoveries. Dr. Schrumpf and his team emphasize a comprehensive approach to pre-operative planning.
Medical Evaluation and Optimization
Before surgery, patients typically undergo a thorough medical evaluation. This process ensures that the patient is healthy enough to tolerate the anesthesia and the procedure itself. Patients must discuss all medications and supplements with their surgeon. Certain medications must be paused for a period of time before surgery. The surgeon will provide a specific timeline for stopping and restarting these drugs.
Physical and Home Preparation
Physical preparation may involve a pre-operative physical therapy program. This program focuses on strengthening the deltoid muscle and maintaining the range of motion in the elbow, wrist, and hand.
Preparing the home environment is an important part of pre-operative planning. Patients will generally need to manage daily tasks with one arm for several weeks. Simple modifications can make a big difference. These include:
- Arranging a recovery area: Set up a comfortable recovery space on the main living level to avoid stairs.
- Accessibility: Place frequently used items at waist level to avoid reaching or bending.
- Bathroom safety: Install a shower chair and grab bars in the bathroom.
- Clothing: Purchase loose-fitting, button-up shirts that are easy to put on and take off.
The Surgical Procedure
The reverse shoulder replacement surgery is a complex, precise operation. It typically takes between one and two hours to complete. The patient receives general anesthesia, often combined with a regional nerve block. The nerve block numbs the shoulder and arm, providing pain control immediately after the surgery.
The surgeon makes an incision, usually on the front or top of the shoulder. The first step involves removing the damaged components. The surgeon then prepares and inserts the artificial components. Finally, the surgeon reduces the joint. This means they place the new humeral socket onto the glenoid ball. The surgeon then closes the incision with sutures or staples. They apply a sterile dressing, and the patient’s arm is placed in a sling.
The Recovery Process: A Phased Approach
Recovery from a reverse shoulder replacement is a journey that requires patience and commitment to a structured rehabilitation program. While timelines and steps may vary, the recovery is generally divided into three main phases.
Phase I: The Immediate Post-Operative Period
This initial phase is primarily focused on protection and pain management. The patient’s arm remains in a sling to protect the healing soft tissues and the newly implanted joint. The block typically provides pain relief for the first 12 to 24 hours. After that, the patient may manage pain with oral medications.
Early Motion: While the joint is protected, gentle, passive range-of-motion exercises begin. Passive motion means the therapist or the patient’s other arm moves the operative arm. The patient does not use their own muscles to move the shoulder. This early, controlled motion is important for preventing stiffness.
Phase II: The Intermediate Phase
Once the surgeon confirms adequate soft tissue healing, the patient transitions to the intermediate phase. The sling is typically discontinued, and the focus shifts to active range of motion.
Active Motion: The patient may now begin to use their deltoid muscle to lift their arm. This is the key functional goal of the reverse replacement. The exercises are still gentle and controlled. The therapist guides the patient to ensure they are using the deltoid muscle effectively.
Light Strengthening: Very light strengthening exercises may begin toward the end of this phase. These exercises focus on isometric contractions, which strengthen the muscle without moving the joint. The patient may also begin to use the arm for light, functional tasks, such as eating and dressing.
Phase III: The Strengthening and Return to Activity Phase
This phase is dedicated to building strength and endurance. The patient works to maximize the functional potential of the new joint.
Progressive Strengthening: The physical therapy program may become more intensive. It incorporates resistance bands, light weights, and functional movements. The focus is on strengthening the deltoid and the muscles around the shoulder blade.
Return to Activity: Many patients can return to driving around the 6- to 8-week mark. By three to six months, patients may typically return to most normal daily activities. Low-impact activities, such as swimming and golf, are often possible. However, the surgeon will frequently advise against high-impact activities or heavy lifting, which could jeopardize the implant’s longevity.
Full recovery, including maximal strength and function, can take six months to a year or longer. It is important to remember that the recovery timeline is highly individual.
Summary
The decision to proceed with a reverse shoulder replacement is a collaborative one between the patient and their orthopedic specialist. For those suffering from the debilitating effects of cuff tear arthropathy or complex fractures, this procedure represents a possible opportunity for pain relief and functional restoration.
The journey involves careful preparation, a precise surgical procedure, and a dedicated commitment to rehabilitation. If you’re struggling with persistent shoulder pain or loss of motion, it may be time to take the next step toward relief. Schedule a consultation with Dr. Schrumpf today to learn whether a reverse shoulder replacement is the right solution for you.