Arthritis is a chronic and often progressive condition characterized by the breakdown of the protective cartilage that cushions the ends of the bones. Shoulder arthritis is a common issue that can limit a person’s ability to perform everyday tasks. Understanding the different forms of shoulder arthritis, the symptoms they present, and the full spectrum of available treatment options is the first step toward management.
Key Takeaways
- Shoulder arthritis is not a single condition. Each type has a distinct cause and progression, which influences the recommended treatment strategy.
- The fundamental problem in most forms of shoulder arthritis is the gradual loss of articular cartilage, the smooth, protective tissue covering the ends of the bones.
- For the majority of patients, initial management focuses on non-surgical, or conservative, treatments. These include activity modification, physical therapy, anti-inflammatory medications, and injections.
- When surgery is necessary, the choice of procedure is highly dependent on the type of arthritis and the condition of the surrounding tissues.
The Anatomy of the Shoulder Joint
Often referred to as the main shoulder joint, the glenohumeral joint is a classic ball-and-socket mechanism. The “ball” is the rounded head of the humerus (upper arm bone), and the “socket” is the shallow, cup-shaped glenoid (part of the shoulder blade, or scapula). This design allows for the incredible mobility of the arm.
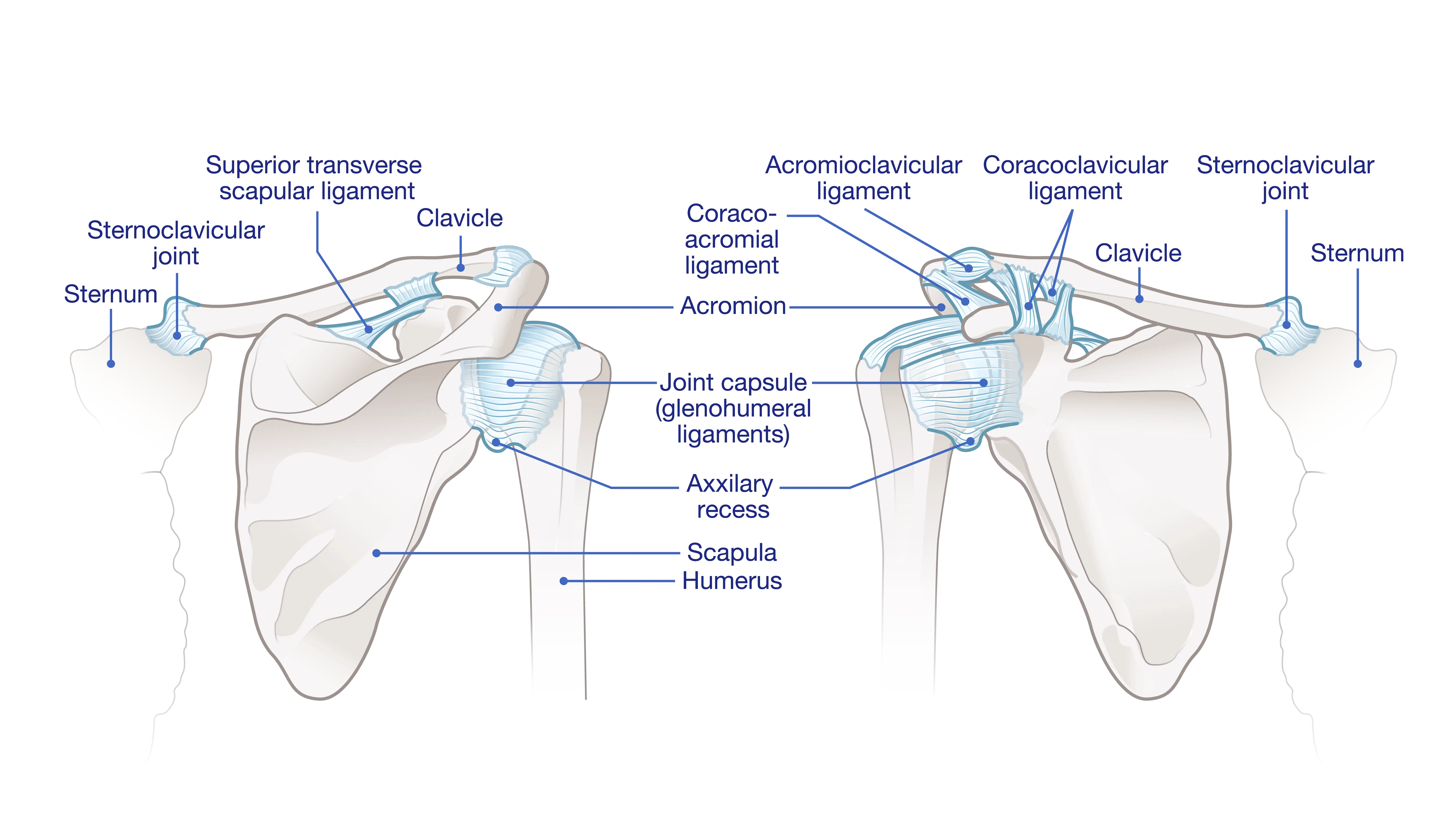
Both the ball and the socket are covered with a layer of smooth tissue called articular cartilage. This cartilage serves two key functions: it provides a nearly frictionless surface for the bones to glide against each other, and it acts as a shock absorber.
The AC joint is located at the top of the shoulder, where the outer end of the clavicle(collarbone) meets the acromion (the highest point of the scapula). While smaller and less mobile than the glenohumeral joint, the AC joint is important for shoulder stability and for allowing the arm to be raised fully overhead. Like the glenohumeral joint, the AC joint also contains cartilage and can be susceptible to arthritic changes.
What is Shoulder Arthritis?
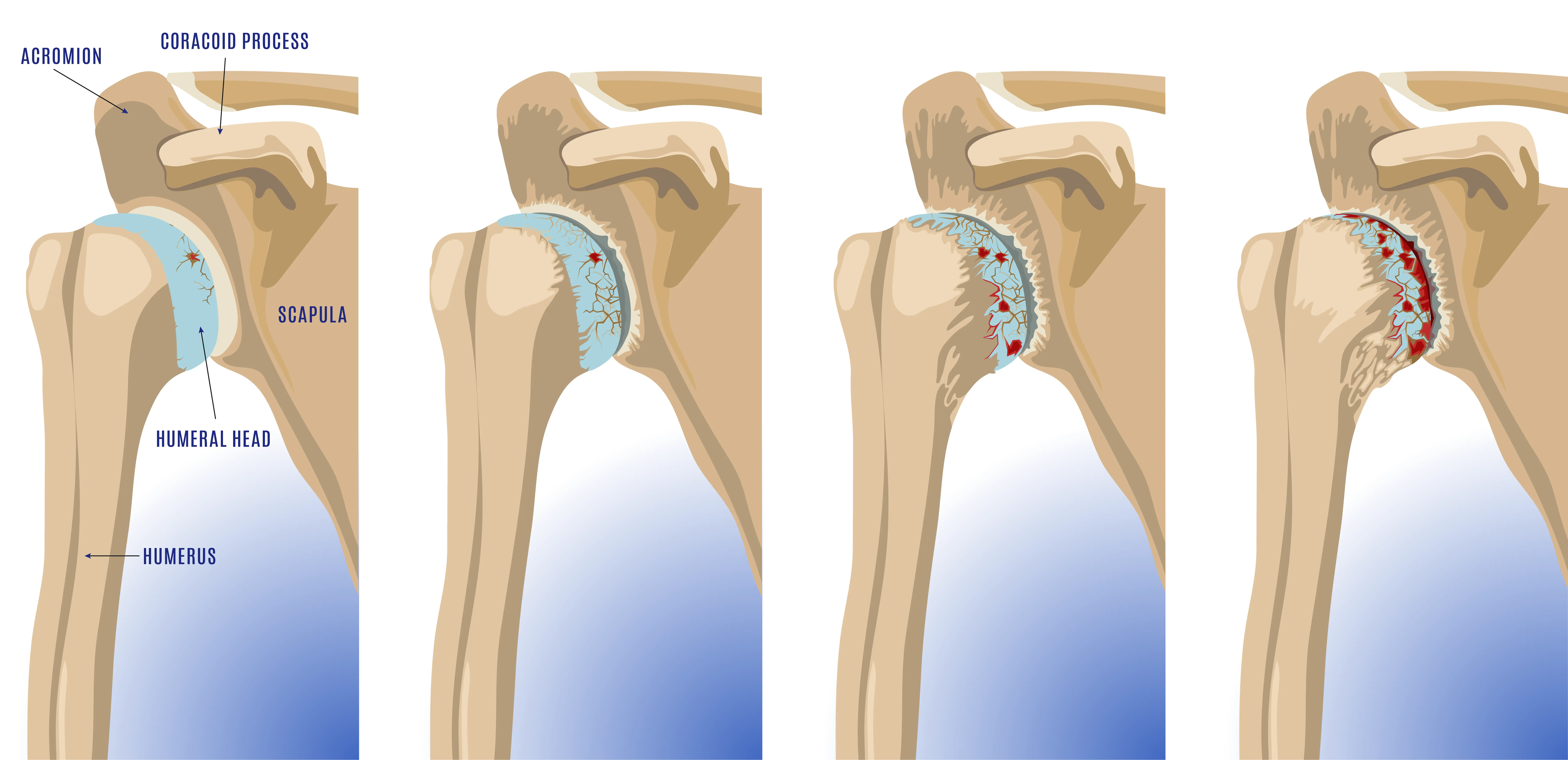
Arthritis in the shoulder is a condition in which the articular cartilage begins to wear away. This process can be slow and gradual, taking many years to develop, or it can be accelerated by injury or other systemic diseases. As the cartilage erodes, the smooth, gliding motion of the joint may be replaced by a rough, grinding motion. In advanced stages, the underlying bone surfaces may rub directly against each other, a condition often described as “bone-on-bone” arthritis. This friction can lead to inflammation, pain, stiffness, and the formation of bony growths called osteophytes(bone spurs) around the joint margins. These osteophytes can further restrict motion and contribute to the overall discomfort.
The Five Major Types of Shoulder Arthritis
Osteoarthritis (OA)
Osteoarthritis, also called “wear-and-tear” arthritis, is the most common form of arthritis and is primarily a mechanical issue related to aging and joint use. It frequently affects individuals over the age of 50. In osteoarthritis, the articular cartilage in the joint gradually breaks down. It is a slow, progressive disease. Symptoms often begin subtly, with pain that is worse after activity or at the end of the day, and stiffness that improves with movement. As the condition advances, pain can become constant, even at rest, and may interfere with sleep.
Rheumatoid Arthritis (RA)
Rheumatoid arthritis (RA) is a systemic, chronic inflammatory disorder. It is classified as an autoimmune disease, meaning the body’s immune system mistakenly attacks its own healthy tissues. RA targets the synovium, the lining of the joint capsule. The immune attack causes the synovium to become inflamed and thickened. This inflamed tissue then releases destructive enzymes that attack and erode the articular cartilage and the underlying bone. Rheumatoid arthritis is typically symmetrical, meaning it usually affects both shoulders.
Post-traumatic Arthritis
Post-traumatic arthritis is a form of osteoarthritis that develops following a significant injury to the shoulder. A severe injury, such as a fracture of the humerus or glenoid, or a shoulder dislocation, can damage the articular cartilage directly. Even if the cartilage is not immediately destroyed, the change in the joint’s mechanics or the presence of fragments can accelerate the normal wear-and-tear process. The onset of symptoms can be delayed, sometimes appearing many years after the initial injury.
Rotator Cuff Tear Arthropathy
This is a form of shoulder arthritis that develops in conjunction with a long-standing rotator cuff tendon tear. The rotator cuff muscles and tendons stabilize the humeral head (the ball) within the glenoid socket. When a large tear is present, the humeral head is no longer held securely in place. Over time, the ball may shift upward and rub against the acromion (the roof of the shoulder). This abnormal contact can wear down the cartilage on the bones.
Avascular Necrosis (AVN)
Avascular necrosis is a condition where the blood supply to the head of the humerus is temporarily or permanently disrupted. Without a consistent blood supply, the bone cells in the humeral head die. This dead bone gradually weakens and collapses, which in turn damages the smooth articular cartilage covering it. The resulting joint destruction can lead to secondary arthritis.
Symptoms, Diagnosis, and Initial Assessment
Recognizing the signs of shoulder arthritis is important for seeking timely medical attention. While symptoms can vary based on the type and severity of the arthritis, several common indicators exist:
- Pain: The most common symptom. It often starts as a dull ache deep within the joint, particularly with movement or activity. As the condition progresses, the pain may become constant, even at rest, and can frequently disrupt sleep.
- Stiffness: A reduced ability to move the shoulder through its full range of motion. This is often most noticeable when trying to reach behind the back or overhead.
- Decreased Range of Motion: The physical limitation of movement.
- Grinding, Clicking, or Catching (Crepitus): A sensation or sound caused by the rough, damaged cartilage surfaces rubbing against each other.
- Weakness: While not always a primary symptom of pure osteoarthritis, weakness is a symptom of rotator cuff tear arthropathy and may also result from pain-related disuse of the muscles.
Diagnosis
The diagnostic process typically begins with a detailed medical history and physical examination. Your doctor may ask about when the pain began, where it is located, how it feels, and whether there have been any previous injuries or related health conditions. During the physical exam, your doctor may evaluate the shoulder’s movement, both when the patient moves it independently and when it is guided, while also checking for tenderness and signs of rotator cuff damage.
Imaging studies are often used to confirm the diagnosis and assess the extent of joint damage. X-rays are usually the first step, revealing joint space, bone spurs, and structural changes such as bone collapse or upward migration of the humeral head. If more detailed bone information is needed, especially for surgical planning, a CT scan may be performed to provide a cross-sectional view of the shoulder. An MRI can offer additional insight into the soft tissues, allowing the doctor to assess the rotator cuff tendons, joint capsule, and other structures not visible on X-ray.
Non-Surgical Treatment Options: The Conservative Approach
Most patients start with non-surgical treatments to reduce pain, limit inflammation, and maintain shoulder mobility. While these approaches may not reverse arthritis, they can help provide relief and potentially delay surgery.
Lifestyle and Activity Changes
Avoiding repetitive overhead movements, heavy lifting, or other painful activities can lessen joint stress. Maintaining a healthy weight supports overall joint health, and small ergonomic adjustments, like raising a computer monitor or using long-handled tools, can help reduce strain.
Physical Therapy
Targeted stretching and strengthening exercises help maintain motion and stabilize the joint. Therapy should be gentle and tailored to avoid irritating the shoulder; exercises that worsen pain should be modified under professional guidance.
Medications
Over-the-counter NSAIDs (such as ibuprofen or naproxen) may reduce pain and inflammation but should be used carefully under medical advice. Acetaminophen is another option for pain relief, especially for those who cannot tolerate NSAIDs.
Heat and Cold Therapy
Ice packs can reduce inflammation and pain after activity, while heat helps ease stiffness and relax muscles, especially in the morning.
Injections
Corticosteroid injections may reduce inflammation and pain for a short period of time but are typically used sparingly to avoid tissue damage. Platelet-rich plasma (PRP) therapy is a regenerative treatment option that involves injecting the patient’s own platelets into the site to help promote healing.
Surgical Treatment Options: When Conservative Care Fails
When non-surgical treatments no longer provide adequate relief or function, surgery may be recommended. The decision is made with an experienced orthopedic surgeon based on the severity of pain, loss of motion, and the specific type of arthritis.
Arthroscopy (Minimally Invasive Surgery)
In early or moderate arthritis, shoulder arthroscopy may be used to smooth damaged cartilage, remove loose fragments, and clean out inflamed tissue. This minimally invasive approach can often ease pain and improve motion, but it does not restore lost cartilage.
Shoulder Replacement (Arthroplasty)
For severe arthritis, replacing the damaged joint surfaces with artificial components may be an effective treatment. The type of replacement depends on the condition of the rotator cuff:
- Total Shoulder Replacement: Generally recommended for patients with advanced arthritis but an intact rotator cuff. The surgeon replaces the humeral head (ball) with a metal implant and resurfaces the socket with a smooth plastic component, replicating the natural anatomy of the shoulder.
- Reverse Shoulder Replacement: Often used when the rotator cuff is severely torn or non-functional. The ball and socket positions are reversed, allowing the deltoid muscle to compensate for the damaged rotator cuff.
Summary
Shoulder arthritis is a complex condition that can deeply affect daily life. Whether caused by the gradual cartilage wear of osteoarthritis or the systemic inflammation of rheumatoid arthritis, successful management requires a thoughtful and personalized approach.
Many patients find meaningful relief through non-surgical measures such as activity modification, physical therapy, and targeted medications or injections. When these methods no longer provide sufficient improvement, surgical treatments, such as total or reverse shoulder replacement, aim to offer pain relief and help restore function.
Frequently Asked Questions
Is shoulder arthritis common, and who is most at risk?
Shoulder arthritis is quite common, particularly osteoarthritis, which affects millions of people worldwide. The risk factors vary by type. For osteoarthritis, the primary risk factors are age (over 50), previous shoulder injuries, and a family history of the condition.
What is the main difference between Osteoarthritis (OA) and Rheumatoid Arthritis (RA) in the shoulder?
OA is a mechanical, “wear-and-tear” condition where the cartilage breaks down over time due to use and age. RA is an autoimmune disease where the body’s immune system attacks the joint lining (synovium). RA is a systemic disease, meaning it affects the entire body, and it is usually symmetrical, affecting both shoulders simultaneously.
What is the “reverse” in Reverse Total Shoulder Replacement?
The “reverse” refers to the anatomical change in the joint. In a natural shoulder and a standard total shoulder replacement, the ball is on the humerus (arm bone) and the socket is on the glenoid (shoulder blade). In a reverse shoulder replacement, this is reversed: a metal ball is placed on the glenoid, and a plastic socket is placed on the humerus. This design is often used when the rotator cuff is severely damaged or non-functional, as it allows the powerful deltoid muscle to lift and move the arm, compensating for the loss of the rotator cuff’s function.






