The shoulder offers the greatest range of motion of any joint in the body. This mobility, however, also makes the joint more vulnerable to injury and degeneration. In the shoulder, arthritis can develop for several distinct reasons. Many patients find themselves asking an important question: What causes arthritis in the shoulder? In this post, we will explore the different types of shoulder arthritis and examine the specific factors that contribute to their development.
Key Takeaways
- The term “arthritis” covers several types. The most common are osteoarthritis, rheumatoid arthritis, and post-traumatic arthritis.
- Osteoarthritis is the most frequent form. It develops as the protective cartilage in the joint gradually wears away over time.
- Your family history and advancing age are non-modifiable risk factors that can predispose you to developing the condition.
- Effective management requires an accurate diagnosis of the specific type and cause of your shoulder arthritis.
Understanding the Shoulder’s Anatomy
The shoulder is a ball-and-socket joint that connects the upper arm bone (humerus) to the shoulder blade (scapula). The “ball” is the head of the humerus. The “socket” is the glenoid, a shallow cup on the scapula.
The ends of both the ball and the socket are covered with articular cartilage. This is a smooth, slippery tissue. Cartilage allows the bones to glide against each other and acts as a shock absorber. Arthritis occurs when this cartilage begins to deteriorate. The bones then may rub directly against each other. This friction creates the characteristic pain and stiffness of the condition.
Osteoarthritis (OA)
Osteoarthritis, often called “wear-and-tear” arthritis, is the most common form. It is a progressive disease where the cartilage in the joint gradually softens and breaks down. This process can happen slowly over many years. As the cartilage erodes, the space between the bones narrows. The body attempts to repair the damage. It does this by growing small, bony spurs called osteophytes, which can further restrict movement.
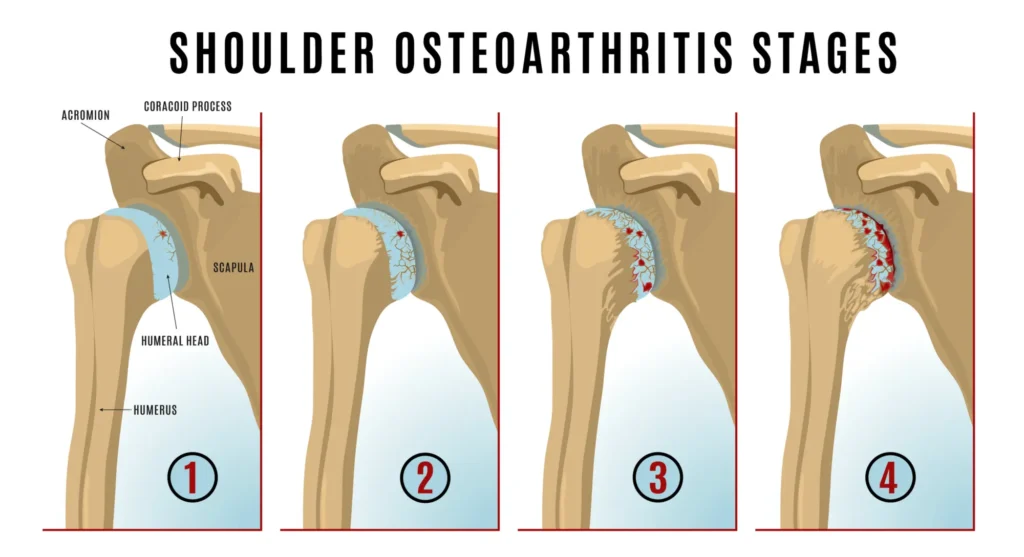
Risk Factors for Shoulder Osteoarthritis
Several factors may increase a person’s risk of developing OA:
- Age: The risk of OA increases with age. Years of use may naturally take a toll on the cartilage.
- Genetics: A family history of osteoarthritis can suggest a genetic predisposition.
- Repetitive Stress: Certain occupations or sports involve repeated, heavy use of the shoulder. This activity may contribute to earlier cartilage breakdown.
Other Types of Shoulder Arthritis
Post-Traumatic Arthritis
This type of arthritis develops after an injury to the shoulder, like a fracture, dislocation, or ligament tear. It may develop many years after the initial event. The injury sets the stage for premature joint degeneration. The body’s healing process may not fully restore the joint’s smooth surface, leading to accelerated wear and tear.
Rheumatoid Arthritis (RA)
Rheumatoid arthritis is an autoimmune condition. This means the body’s immune system mistakenly attacks its own healthy tissues. In RA, the immune system targets the lining of the joint capsule (synovium). The resulting inflammation causes the synovium to swell. This swollen tissue then releases chemicals that can destroy the cartilage and bone. RA often affects both shoulders at the same time.
Rotator Cuff Tear Arthropathy
This is a complex form of shoulder arthritis. It develops after a massive, long-standing tear of the rotator cuff tendons. The rotator cuff is a group of muscles and tendons that help to stabilize and move the shoulder. A large tear compromises the stability of the joint. The humerus head moves upward and rubs against the acromion (the top part of the shoulder blade). This abnormal rubbing can cause damage to the cartilage.
Avascular Necrosis
Avascular necrosis, or osteonecrosis, occurs when the blood supply to the head of the humerus is disrupted. Bone tissue needs a constant blood supply to stay healthy, so without blood, the bone can collapse. This damages the cartilage covering it.
Risk Factors That Influence Arthritis Development
The specific type of arthritis provides a direct answer to what causes arthritis in the shoulder. However, several underlying factors may also influence arthritis development.
Biomechanical Factors
The way your shoulder moves and is aligned plays a role:
- Joint Instability: Chronic instability, even subtle forms, causes the joint surfaces to grind unevenly. This uneven pressure may accelerate cartilage wear.
- Improper Healing: After a fracture, the joint surface may be permanently altered. This can create a rougher, less efficient joint.
Systemic and Lifestyle Factors
Your overall health and habits also contribute to joint health.
- Obesity: While less direct than in weight-bearing joints like the knee, excess body weight may increase systemic inflammation.
- Metabolic Conditions: Conditions like diabetes may affect the health of connective tissues. This could potentially make cartilage more vulnerable to damage.
Recognizing the Symptoms of Shoulder Arthritis
Pain is the most common symptom. It is frequently experienced deep within the joint and may radiate down the arm. The pain may worsen with activity, and many patients experience pain at night that interferes with sleep.
The shoulder loses its flexibility. Patients may find it difficult to lift their arm, and simple tasks like reaching overhead or behind the back can become challenging. Additionally, patients may experience a grinding, clicking, or catching sensation known as crepitus. Muscle weakness can also develop if the pain limits movement. The surrounding muscles then become deconditioned.
Diagnosis and Treatment Overview
If you are experiencing symptoms, it may be time to consider consulting an experienced shoulder specialist to evaluate the condition and help guide diagnosis and treatment.
During the physical exam, your range of motion and strength may be assessed. Imaging tests may be used to support the diagnosis. Standard X-rays are the primary diagnostic tool. They can often show the extent of cartilage loss and reveal the presence of bone spurs. Magnetic resonance imaging (MRI) may be used to help evaluate the condition of the rotator cuff tendons.
Treatment Options
Treatment aims to reduce pain and restore function, and initial treatment is frequently non-surgical:
- Physical Therapy: Specific exercises may be recommended to help maintain motion and strengthen surrounding muscles.
- Medication: Non-steroidal anti-inflammatory drugs (NSAIDs) may help manage pain and reduce inflammation.
- Injections: Corticosteroid injections may provide temporary pain relief.
When non-surgical treatments fail, surgical options may be recommended. These may include arthroscopy for early cases or, for advanced cases, total shoulder replacement or reverse shoulder replacement.
Summary
Shoulder arthritis is a complex condition, with multiple potential origins. The question of “what causes arthritis in the shoulder?” has several answers. Osteoarthritis results from long-term mechanical wear. Post-traumatic arthritis stems from a past injury. Rheumatoid arthritis is an autoimmune response. Rotator cuff tear arthropathy is a possible consequence of rotator cuff damage.
Frequently Asked Questions
Can I prevent shoulder arthritis?
Not all forms of shoulder arthritis can be prevented. You can, however, reduce your risk. Prevention strategies may include maintaining a healthy weight, avoiding repetitive, heavy overhead lifting when possible, and promptly treating any shoulder injuries.
When should I consider surgery for shoulder arthritis?
Surgery is typically considered when non-surgical treatments no longer provide adequate pain relief. Your surgeon will evaluate your specific condition and can recommend the most appropriate surgical option, such as arthroscopy or total or reverse shoulder replacement.
What is the difference between total and reverse shoulder replacement?
A total shoulder replacement (anatomic) is most often used when the rotator cuff is healthy. It replaces the ball and socket with prosthetic components, replicating the natural anatomy. A reverse shoulder replacement is frequently used when the rotator cuff is severely damaged. It reverses the position of the ball and socket, which allows the deltoid muscle to compensate for the non-functional rotator cuff.






