Shoulder pain from arthritis can gradually turn everyday tasks into challenges. Reaching for a coffee mug, getting dressed in the morning, or even finding a comfortable sleeping position may become difficult as the joint’s protective cartilage wears down over time. When conservative treatments such as physical therapy, medications, and injections no longer provide adequate relief, shoulder arthritis surgery may be considered to help reduce pain and improve function. In this post, we’ll review the primary surgical options, what to expect from the treatment process, and how advances in implant technology and surgical planning are supporting improved patient outcomes.
Key Takeaways
- Shoulder arthritis develops when the cartilage lining the joint wears down, leading to pain and limited mobility.
- When conservative care no longer provides adequate relief, shoulder arthritis surgery may be recommended by your orthopedic surgeon.
- Total shoulder replacement (anatomic shoulder arthroplasty) replaces the worn joint surfaces and is often recommended for patients with an intact rotator cuff.
- Reverse shoulder replacement uses a different implant configuration and may be recommended when the rotator cuff is significantly damaged or irreparable.
Understanding Shoulder Arthritis
Your shoulder is a ball-and-socket joint. The upper part of the arm bone (the humerus) forms the ball, and a part of the shoulder blade (the scapula) called the glenoid forms the socket. Both surfaces are covered in a smooth layer of articular cartilage that helps the joint move freely and without pain.
Shoulder arthritis develops when that cartilage gradually wears down. Over years of use, the smooth lining thins and may eventually deteriorate to a point where movement becomes painful and less efficient. You might notice a deep ache in the joint, stiffness that gets worse over time, and a grinding or clicking sensation during movement.
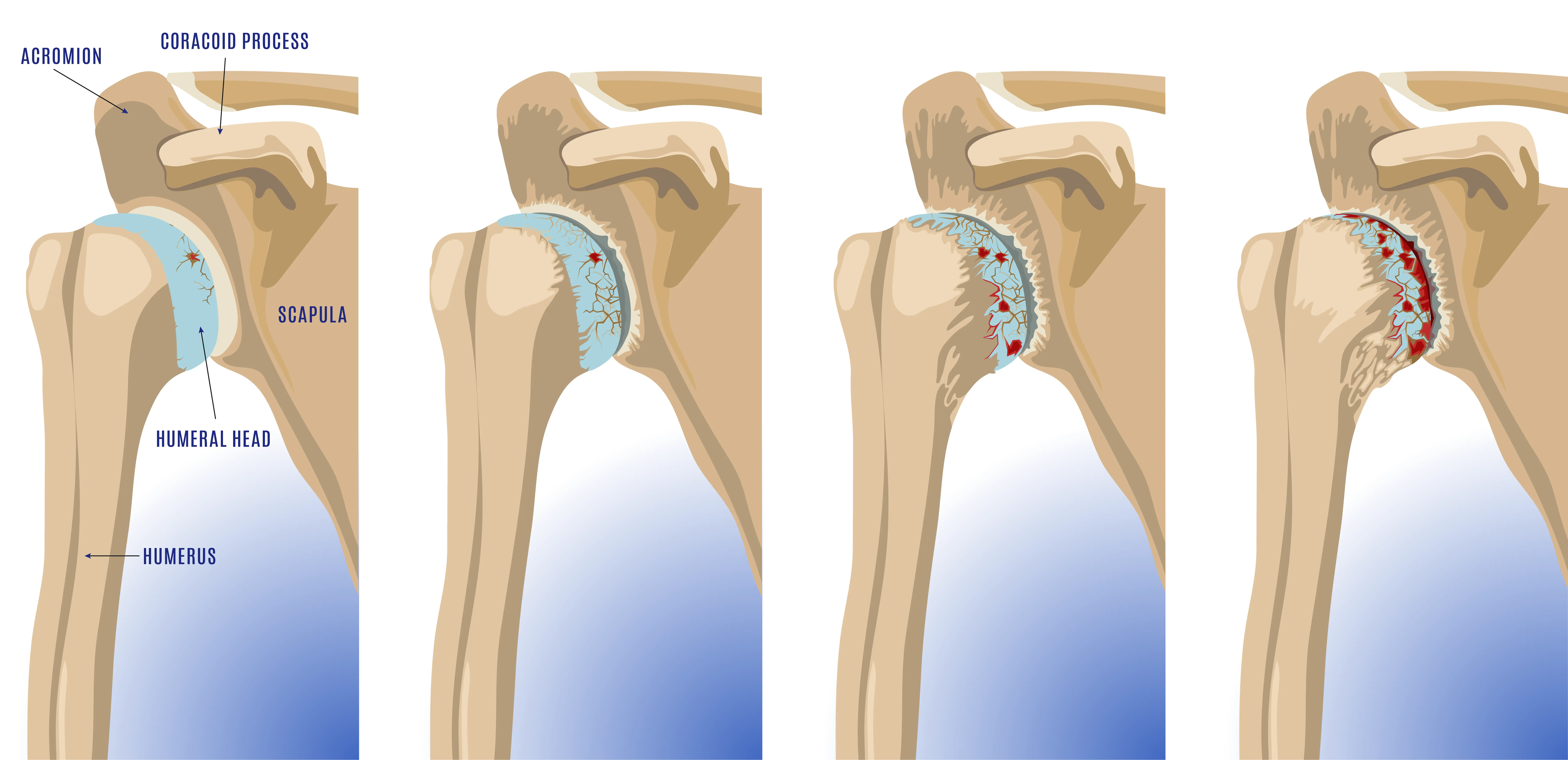
The most common form is osteoarthritis, which results from gradual wear and tear. Rheumatoid arthritis, where the body’s immune system attacks the cartilage, is less common but can also affect the shoulder. Post-traumatic arthritis may develop after a previous shoulder injury, such as a fracture or a torn rotator cuff, that changes the way the joint surfaces interact over time.
When Is It Time to Consider Shoulder Arthritis Surgery?
Surgery is generally not the first step. Many shoulder specialists will recommend a progression of non-surgical treatments before discussing surgical options.
Physical therapy is often a component of early treatment. A skilled therapist can help you maintain range of motion, strengthen the muscles around the shoulder, and reduce pain. Activity modification, adjusting how you use your shoulder during daily tasks or exercise, can also make a difference. When pain persists, nonsteroidal anti-inflammatory medications (NSAIDs) or corticosteroid injections may offer temporary relief.
However, arthritis tends to progress. There may come a point when these conservative measures no longer provide enough relief to maintain your quality of life. If shoulder pain is disrupting your sleep, making it hard to get dressed, or preventing you from enjoying activities like golf, tennis, or gardening, your surgeon may recommend shoulder arthritis surgery. The goal is to reduce pain and improve functional movement so you can return to the activities that matter most to you.
Total Shoulder Replacement Surgery
Total shoulder replacement, also called total shoulder arthroplasty or anatomic shoulder replacement, is one of the most well-established surgical treatments for severe shoulder arthritis. During this procedure, a surgeon replaces the damaged joint surfaces with prosthetic components designed to replicate the natural shape and function of your shoulder.
Total shoulder replacement tends to work well for patients whose rotator cuff is still intact and functional. The rotator cuff is a group of tendons and muscles that stabilize and move the shoulder joint. A total shoulder replacement aims to deliver pain relief and improved range of motion when the rotator cuff is healthy.
After maximal recovery, many patients find they can return to daily activities and even recreational pursuits like golf and swimming. Results vary by individual, of course, but the potential for meaningful improvement in quality of life is one of the primary reasons this surgery remains so popular.

Reverse Shoulder Replacement Surgery
Reverse shoulder replacement may be recommended when shoulder arthritis is accompanied by a large, irreparable rotator cuff tear, a condition sometimes called cuff tear arthropathy (CTA).
In a healthy shoulder, the ball sits on the humerus and the socket is on the scapula. A reverse shoulder replacement changes that orientation. A reverse shoulder replacement flips that arrangement. The ball component is placed on the glenoid (socket side), and the socket component is placed on the humeral (arm bone) side.
When the rotator cuff is severely damaged, it can no longer stabilize and move the shoulder effectively. A traditional total shoulder replacement relies on a functioning rotator cuff to work properly. The reverse design, however, allows the deltoid muscle, the large muscle covering the outside of the shoulder, to compensate and power the arm’s movement.
Reverse shoulder replacement may also be recommended for other conditions, including complex shoulder fractures. Your surgeon will evaluate your individual anatomy, condition, and lifestyle to determine which type of replacement is likely the best fit.

The Role of Modern Implant Technology
Shoulder replacement surgery has advanced considerably over the past few decades. Implant design, materials, and surgical planning tools have all improved, and these developments are helping surgeons tailor procedures to each patient’s unique anatomy.
One example is the InSet® Shoulder System from Shoulder Innovations. For anatomic total shoulder replacement, this system offers both short-stem and stemless humeral implant options. Providing multiple configurations allows surgeons to select an implant that aligns more closely with a patient’s individual bone quality, anatomy, and surgical goals. The system’s glenoid design is intended to sit more within the native bone rather than on top of it, which may help reduce the mechanical stresses that can contribute to glenoid loosening.
For reverse shoulder replacement, the InSet® Reverse System offers an extensive selection of component options. This flexibility can help surgeons tailor-fit the implant to each patient’s unique condition, which may improve shoulder motion outcomes and help reduce the risk of certain complications.
Another meaningful advancement is the use of computerized surgical planning. Software like ProVoyance® converts a patient’s CT scan into a three-dimensional digital model of their shoulder. Surgeons can then evaluate the bone structure virtually and plan the optimal placement and alignment of the implant before stepping into the operating room. This level of preoperative planning may support more precise implant positioning and thoughtful surgical execution, which can be important factors in long-term performance.
Preparing for Shoulder Arthritis Surgery
If you and your surgeon decide that shoulder arthritis surgery is the right step, preparation plays an important role in setting the stage for a smooth experience. Your surgical team will likely guide you through a preoperative checklist tailored to your specific needs.
Setting up your home for recovery ahead of time can make a big difference. Simple changes like moving frequently used items to counter height, arranging a comfortable sleeping area, and having loose-fitting clothing ready can ease those first few weeks. Many patients also find it helpful to arrange for someone to assist with daily tasks during the initial recovery period.
What to Expect During Recovery
Recovery from shoulder replacement surgery is a gradual process. Every patient’s experience is a little different, but understanding the general timeline can help you set realistic expectations.
In the first few weeks, your arm will typically be supported in a sling. Pain management during this phase is a priority, and your surgical team will work with you to keep discomfort under control. Gentle, guided exercises may begin relatively early to help prevent stiffness and promote healing.
A structured rehabilitation program helps restore strength, flexibility, and range of motion over the weeks and months following surgery. Many patients begin to notice meaningful improvements in pain and function within the first three to six months, though maximal recovery can take up to a year or more in some cases.
Life After Shoulder Replacement
One of the most encouraging aspects of shoulder replacement surgery is the potential for a return to daily activities and hobbies. Many patients report that they can once again sleep comfortably, reach overhead, get dressed without pain, and participate in recreational activities they had given up.
That said, certain high-impact activities may need to be avoided or modified to protect your new joint. Your surgeon will provide specific guidance based on your procedure and your body’s response to surgery. Low-impact activities such as swimming, golf, and gardening are often well-tolerated, though recommendations may vary depending on your individual case. Contact sports or heavy repetitive lifting may be discouraged.
Choosing the Right Surgeon
Selecting an experienced shoulder surgeon who specializes in shoulder replacement can make a significant difference in your experience and outcomes. Look for a board-certified orthopedic surgeon with specific training and expertise in shoulder arthroplasty.
Don’t hesitate to ask questions during your consultation. You might ask about the surgeon’s experience with your specific condition, the type of implant they recommend and why, and what their patients typically experience during recovery. A good surgeon will take the time to listen to your concerns, explain your options clearly, and help you feel confident in your treatment plan.
Summary
Shoulder arthritis surgery continues to evolve. Today’s patients have access to refined surgical techniques, personalized implant options, and advanced planning tools that may help support improved outcomes. Whether total shoulder replacement or reverse shoulder replacement is right for you depends on your specific condition, the health of your rotator cuff, and your individual goals.
The most important step is starting a conversation with a qualified shoulder specialist. Together, you can evaluate your options, weigh the potential benefits and risks, and develop a plan that makes sense for your life. Shoulder arthritis surgery is a significant decision, but for many patients, it represents a meaningful opportunity to reduce pain, restore function, and reclaim the activities that matter most.
Frequently Asked Questions
How do I know if I need shoulder arthritis surgery?
If non-surgical treatments like physical therapy, medications, and injections are no longer controlling your shoulder pain, and your daily activities are significantly affected, it may be time to discuss surgical options with an orthopedic surgeon. Your doctor will evaluate your imaging, medical history, and functional limitations to help determine whether shoulder arthritis surgery could be beneficial.
What is the difference between a total shoulder replacement and a reverse shoulder replacement?
A total (or anatomic) shoulder replacement replaces the damaged joint surfaces while maintaining the natural ball-and-socket orientation. A reverse shoulder replacement switches the ball and socket positions, allowing the deltoid muscle to power arm movement. It may be recommended when the rotator cuff is severely torn or irreparable.
Will I be able to return to sports and activities after surgery?
Many patients can return to low-impact activities such as golf, swimming, and gardening after shoulder replacement. Higher-impact or contact sports may need to be limited. Your surgeon will provide personalized recommendations based on your specific procedure and recovery progress.






